Posted by: Atlantic Eye Institute in Education
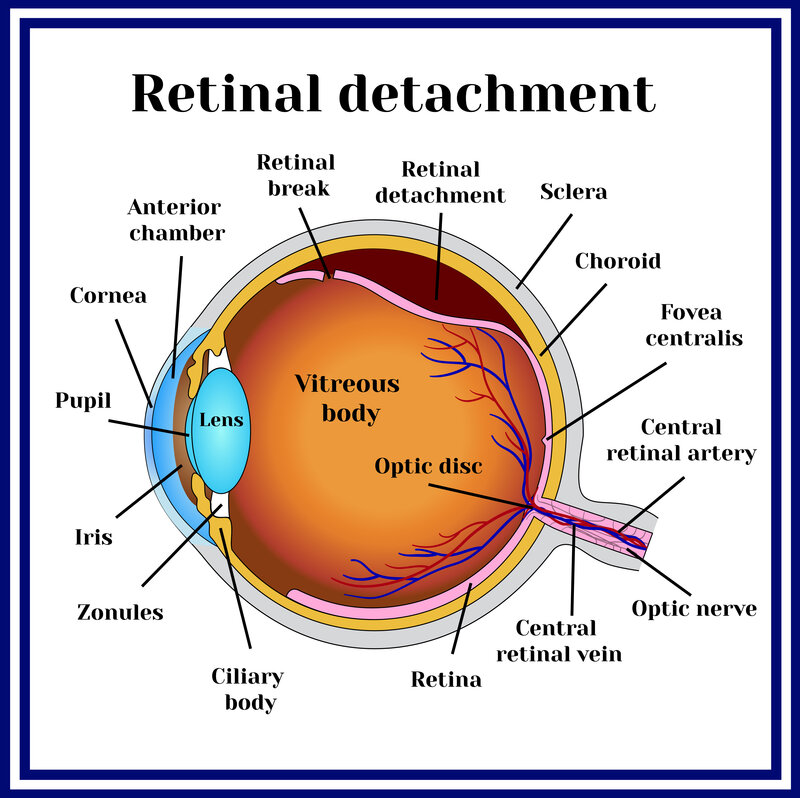
The retina is a light-sensitive layer attached to the rear of the eyeball. It converts light signals into electrical signals, which the optic nerve travels to the brain – forming an image.
Sometimes, the retinal layer detaches from the eyeball – called retinal detachment. When this occurs, it deprives retina tissue from healthy circulation. Over time, the combination of a change in retinal shape and the deterioration of the starved tissue causes increasing vision loss.
Without immediate treatment, a detached retina worsens and can eventually cause irreversible vision loss.
Signs & Symptoms Of Retinal Detachment
Surprisingly, detached retinas are not painful and don’t typically cause any physical sensations at all. As a result, patients often ignore the signs, especially if symptoms are mild, risking further detachment, the need for more complicated treatment, or even permanent vision loss.
Proactive eye care and healthy lifestyle treatments are a sound foundation for avoiding retinal detachment. Small tears may not cause any symptoms at all, although the tissue is compromised and becomes increasingly damaged. If you have a small retinal tear, we’ll notice it at your annual eye exam. However, we also recommend learning the signs or symptoms so you can schedule an eye appointment as early as possible.
Here are some of the most common signs of retinal detachment:
Lots of new floaters
Seeing floaters isn’t all that uncommon. We all get floaters occasionally, appearing like little dots or squiggles. In most cases, floaters are perfectly normal, and nothing needs to be done (despite their annoyance). However, because they’re a sign of a detached retina, we always recommend scheduling an appointment if you experience more than the occasional floater in your field of vision.
Flashes of light in one or both eyes
Since translating light into electrical signals is the retina’s job, it makes sense that torn or detached retinas can’t do their job properly. This can result in mixed or incorrect signaling, and patients may experience light flashes. Most patients relate this experience to “seeing stars” after you’re hit in the eye by a ball or blunt object.
Again, a short, solo flash of light or a random “spark” isn’t much to worry about. However, seeing regular flashes of light deserves a call to the optometrist.
Shadows in your peripheral vision
More severe detachment can result in shadowy peripheral vision – meaning you have a sort of tunnel vision. Due to patient descriptions, we refer to this as the “curtain symptom” because it can feel like your central vision is the stage, and curtains are blocking the view of each “side” of the stage. Any change in peripheral vision should be investigated.
General curtain effect
Other times, it may seem like a curtain is descending on a particular portion of your visual field rather than the peripheral. How you experience symptoms is always related to where the retina detaches and how large of a portion is pulled away from the eyeball.
Risk Factors For Retinal Detachment
Sometimes, we aren’t sure why the retina tears or detaches from the rear wall of the eye. However, certain factors elevate the risks. These are:
- Eye trauma
- Being extremely nearsighted (people who need glasses or contacts to see distance are more likely to develop detached retinas than those who are farsighted and only need reading glasses) or having degenerative myopia.
- Genetic predisposition (someone in your immediate family has had them before, or you’ve experienced it in the past).
- You’ve had eye surgery (cataract, glaucoma, etc.).
- Diabetic retinopathy.
- Posterior vitreous detachment.
- Other eye diseases, like retinoschisis or lattice degeneration.
Don’t forget that a healthy lifestyle is the foundation of good health – including vision health – and can reduce your chances of experiencing a detached retina. If you have a detached retina, we’ll use the treatment that works best with the severity and your overall health.
Treating Torn & Detached Retinas
The goal of any treatment is to reattach the detached portion to the rear of the eye wall, simultaneously treating any tears or holes. There are several different options:
Pneumatic retinopexy (gas bubble treatment)
This procedure takes place right in our office. We inject a gas bubble into the eye. The location and pressure from the bubble help to push the retina back into place. When caught early enough, and when tissues are still healthy, the retina slowly reattaches to the eye wall.
Once the procedure is complete, you must keep your head in a very specific position for at least a few days. We’ll provide instructions on how to prepare for that. Throughout the healing period, the body produces fluid that replaces the gas bubble, exerting accurate pressure to help keep the retina in place.
Vitrectomy
During this procedure, the ophthalmologist removes the vitreous humor that’s pulling on the retina with a bubble (gas, air, or oil). If the best option is oil, the oil bubble will be removed in a few months. If the best choice is gas or air, you must avoid certain activities (both at altitude or under the water) to avoid pressure expansion until it’s completely healed.
Scleral buckle
With the first two options, we insert bubbles that put pressure on the retina internally to push it back against the rear wall of the eye. With a scleral buckle procedure, we sew a soft plastic belt or band around the exterior of the eye. It pushes the affected tissue inward, helping it meet the separated retina. In most cases, the scleral buckle is permanently left in place.
As with any surgery, there are pros and cons, including inherent risks – like infection, bleeding, excess pressure, etc. We discuss all of the risks and benefits with you beforehand so you can make an informed choice.
Atlantic Eye Institue Has Board-Certified Optometrists & Opthalmomoligists
Here at Atlantic Eye Institute, we have board-certified optometrists and ophthalmologists who diagnose and treat torn or detached retinas. We’re a one-stop destination for any issues affecting eye and vision health.
Are you currently experiencing signs or symptoms of retinal detachment? Schedule your appointment today. Otherwise, schedule appointments every year so we can catch any red flags at the very first opportunity, which is always the best recipe for treatment success.



